Understanding Alternative Healthcare Options in Australia: A Comprehensive Patient Guide
Introduction: The Evolving Landscape of Australian Healthcare
Australia’s healthcare landscape has undergone significant transformation over the past decade, with patients increasingly seeking information about the full spectrum of healthcare options available to them. This comprehensive guide explores alternative healthcare pathways within the Australian medical system, providing patients with the knowledge needed to make informed decisions about their healthcare journey while understanding the regulatory frameworks that govern these options.
The term “alternative healthcare” encompasses a broad range of therapeutic approaches that may complement or provide alternatives to conventional medical treatments. In Australia, these options operate within a carefully structured regulatory environment designed to ensure patient safety while preserving access to diverse healthcare modalities.
Understanding this landscape requires familiarity with:
- The roles of various regulatory bodies
- The categories of alternative treatments available
- The legal pathways through which patients may access these options
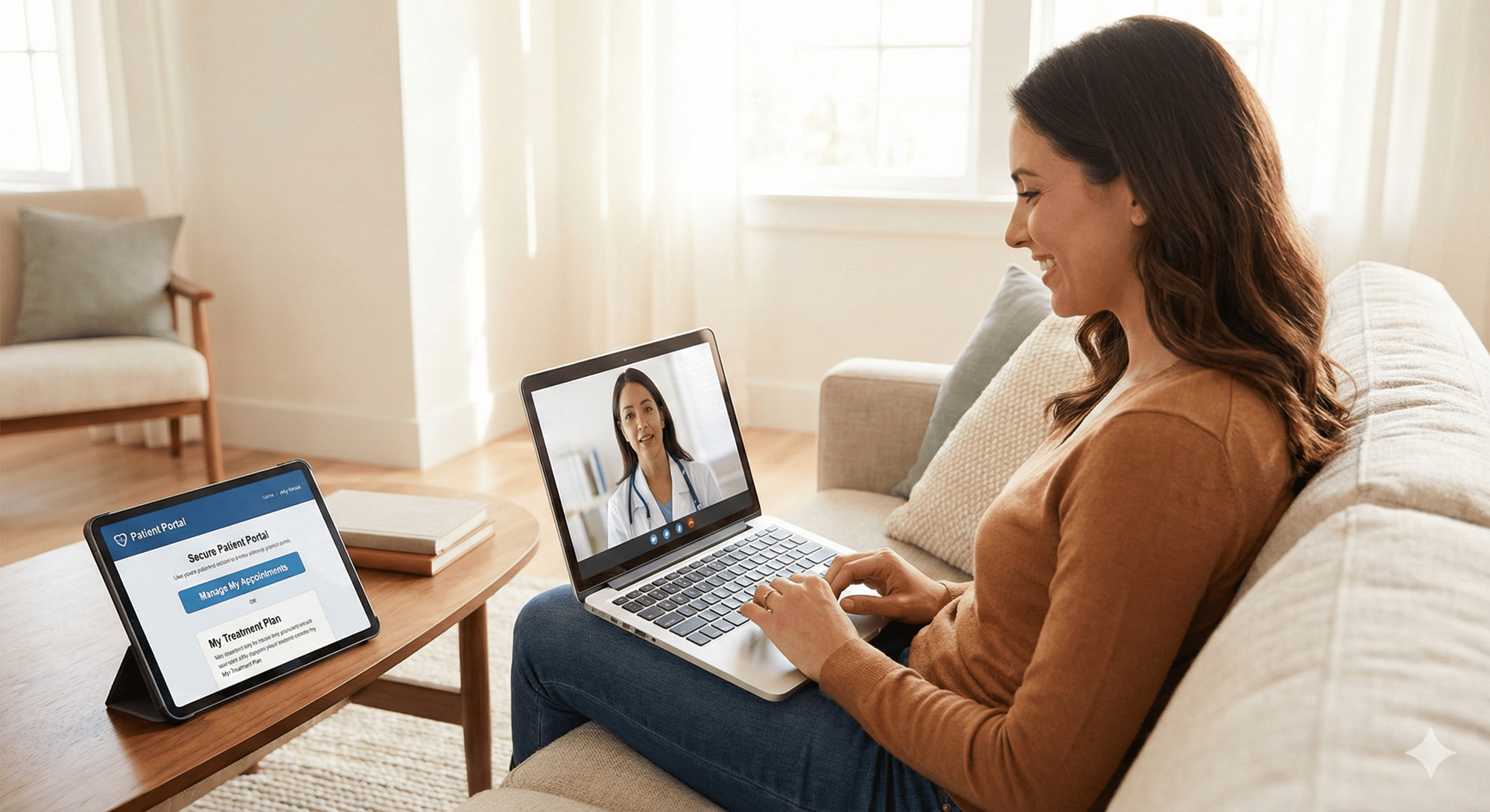
The rise of telehealth has fundamentally changed how patients interact with healthcare providers, including those offering alternative healthcare services. Telehealth consultations now enable patients across Australia, including those in rural and remote areas, to access specialised healthcare expertise that was previously available only in major metropolitan centres. This development has particular relevance for alternative healthcare, where specialist practitioners may be concentrated in specific locations.
This guide will:
- Explain the fundamentals of alternative healthcare in Australia
- Describe the regulatory frameworks that protect patients
- Outline the role of telehealth in expanding healthcare access
- Provide practical information about how to explore these options through appropriate medical channels
Our goal is to empower you with knowledge while emphasising that all healthcare decisions should involve consultation with qualified medical practitioners.

Something Powerful
Tell The Reader More
The headline and subheader tells us what you're offering, and the form header closes the deal. Over here you can explain why your offer is so great it's worth filling out a form for.
Remember:
- Bullets are great
- For spelling out benefits and
- Turning visitors into leads.
What Is Alternative Healthcare? Understanding the Terminology
Defining Alternative and Complementary Medicine
Alternative healthcare refers to therapeutic approaches that fall outside the scope of conventional Western medicine, or that may be used alongside conventional treatments in what is often termed “integrative” or “complementary” medicine.
The World Health Organization recognises traditional and complementary medicine as an important part of healthcare systems worldwide, and Australia has developed specific regulatory frameworks to govern these practices.
It is important to understand the distinction between several related terms:
- Alternative medicine – approaches used instead of conventional medical treatment
- Complementary medicine – approaches used alongside conventional treatment
- Integrative medicine – a coordinated approach that combines conventional and complementary treatments in a structured way
In practice, many healthcare providers in Australia take an integrative approach, working with patients to develop comprehensive care plans that may incorporate multiple therapeutic modalities.
Categories of Alternative Healthcare Options
Alternative healthcare in Australia encompasses several distinct categories, each with its own regulatory considerations and access pathways. Understanding these categories helps patients navigate the healthcare landscape more effectively and engage in informed discussions with healthcare providers.
1. Plant-Based and Botanical Medicine
This category includes therapeutic approaches derived from plant sources. In Australia:
- Some plant-derived substances have been incorporated into conventional medicine (such as certain pharmaceutical preparations)
- Others remain within the alternative or complementary medicine sphere
- Access to certain plant-based medicines may be restricted and require specific approval pathways through the Therapeutic Goods Administration (TGA)
2. Traditional Medicine Systems
These include established systems such as:
- Traditional Chinese Medicine (TCM)
- Ayurveda
- Indigenous Australian healing practices
Many of these systems have been practised for thousands of years and continue to serve millions of people worldwide. In Australia, practitioners of some traditional medicine systems are regulated under state and territory laws.
3. Mind–Body Interventions
This category includes practices such as:
- Meditation
- Yoga
- Mindfulness-based approaches
While these are often considered wellness practices rather than medical treatments, they may be incorporated into comprehensive healthcare plans and are increasingly recognised by conventional healthcare providers.
4. Manipulative and Body-Based Practices
This includes:
- Chiropractic
- Osteopathy
- Massage therapy
In Australia, chiropractors and osteopaths are regulated health professions, with practitioners required to be registered with the Australian Health Practitioner Regulation Agency (Ahpra).
5. Nutritional and Dietary Approaches
This encompasses:
- Dietary modifications
- Nutritional supplementation
- Specialised diets that may be recommended as part of a healthcare plan
While general dietary advice is available from various sources, specific nutritional interventions should be supervised by qualified healthcare practitioners.
The Australian Regulatory Framework for Healthcare
Australia maintains one of the world’s most comprehensive healthcare regulatory systems, designed to ensure patient safety while enabling access to a wide range of therapeutic options. Understanding this framework is essential for patients seeking to navigate alternative healthcare pathways legally and safely.
The regulatory environment involves multiple agencies working together to oversee different aspects of healthcare delivery.
The Therapeutic Goods Administration (TGA)
The Therapeutic Goods Administration (TGA) is Australia’s regulatory authority for therapeutic goods, including:
- Medicines
- Medical devices
- Biological products
The TGA operates under the Therapeutic Goods Act 1989 and is responsible for evaluating, assessing and monitoring products to ensure they meet appropriate standards of quality, safety and efficacy.
Under the TGA framework, medicines are classified into schedules that determine how they may be accessed:
- Schedule 2 – Pharmacy medicines (available only from pharmacies)
- Schedule 3 – Pharmacist-only medicines
- Schedule 4 – Prescription-only medicines (require a prescription from a medical practitioner)
- Schedule 8 – Controlled drugs with strict access requirements due to their potential for misuse or dependence
This scheduling system ensures that medicines with greater potential risks are accessed only under appropriate medical supervision.
For alternative healthcare options that involve therapeutic goods, the TGA’s regulatory framework determines:
- Whether products are approved for supply in Australia
- The circumstances under which they may be accessed
Some therapeutic goods used in alternative healthcare may not be approved for general supply in Australia but may be accessed through specific pathways such as the:
- Special Access Scheme (SAS)
- Authorised Prescriber Scheme
Australian Health Practitioner Regulation Agency (Ahpra)
Ahpra works with National Boards to regulate health practitioners in Australia. The agency’s primary role is to protect the public by ensuring that only health practitioners who are suitably trained and qualified to practise in a safe and competent manner are registered.
Ahpra:
- Maintains a public register of all registered health practitioners
- Enables patients to verify the credentials of healthcare providers
For patients exploring alternative healthcare options, Ahpra registration provides assurance that practitioners meet national standards for education, training and professional conduct. Registered practitioners are:
- Bound by professional codes of conduct
- Subject to oversight regarding their clinical practices
This includes practitioners who may offer alternative healthcare services alongside, or as part of, conventional medical practice.
Ahpra has developed specific guidelines for telehealth practice, which have particular relevance given the growing role of remote consultations in alternative healthcare. These guidelines emphasise that:
- Telehealth consultations must meet the same standards of care as in-person consultations
- Practitioners must ensure they have adequate information to provide appropriate clinical advice
State and Territory Health Departments
In addition to federal regulation through the TGA and Ahpra, state and territory health departments maintain their own regulatory requirements for certain healthcare activities. These may include:
- Additional requirements for the prescription or supply of certain therapeutic goods
- Licensing requirements for healthcare facilities
- Public health regulations that may affect the delivery of alternative healthcare services
Patients should be aware that access to certain alternative healthcare options may vary between states and territories due to these jurisdictional differences. Healthcare providers operating legally within the Australian system will be familiar with the requirements applicable in their jurisdiction and can advise patients about any state-specific considerations.
Legal Access Pathways for Alternative Healthcare
Understanding how to legally access alternative healthcare options is crucial for patients. Australia’s regulatory framework provides several pathways through which patients may access therapeutic goods and services, including those that may not be generally available through standard channels. These pathways maintain appropriate medical oversight while enabling access to treatments that may benefit patients under appropriate circumstances.
Conventional Medical Consultation
The primary pathway for accessing healthcare in Australia is through consultation with a registered medical practitioner.
- General practitioners (GPs) serve as the first point of contact for most patients
- GPs can provide referrals to specialists when needed
This pathway applies equally to discussions about alternative healthcare options. Patients may discuss their interest in alternative approaches with their GP, who can:
- Provide medical advice
- Facilitate access to alternative treatments through proper channels where appropriate
Medical practitioners are bound by professional standards that require them to:
- Provide care based on the best available evidence
- Act in their patients’ best interests
This means practitioners will consider requests for alternative healthcare options within the context of each patient’s individual circumstances, including:
- Medical history
- Current health status
- Treatment goals
Practitioners may:
- Recommend against certain options if they believe the risks outweigh potential benefits, or
- Support access to appropriate treatments through established legal pathways
Specialist Alternative Healthcare Clinics
In recent years, specialised clinics have emerged in Australia that focus specifically on alternative healthcare options. These clinics typically:
- Operate with medical practitioners who have developed expertise in specific areas of alternative medicine
- Understand the regulatory pathways for accessing treatments that may not be generally available
Patients may access these clinics:
- Through referral from their GP, or
- In some cases, through direct booking
When considering a specialist alternative healthcare clinic, patients should:
- Verify that the clinic employs appropriately qualified and registered healthcare practitioners
- Use the Ahpra public register to confirm practitioner registration
Legitimate clinics will be transparent about:
- Their practitioners’ qualifications
- The regulatory frameworks under which they operate
Special Access Scheme (SAS)
The Special Access Scheme (SAS) provides a legal pathway for medical practitioners to access unapproved therapeutic goods for individual patients on a case-by-case basis. This scheme is particularly relevant for certain alternative healthcare options that involve therapeutic goods not included in the Australian Register of Therapeutic Goods (ARTG).
The SAS operates in several categories:
SAS Category A
- Allows medical practitioners to supply certain unapproved goods to patients who are seriously ill with a condition from which they are expected to die within a short period
- Has specific eligibility requirements and reporting obligations
SAS Category B
- Requires medical practitioners to apply to the TGA for approval to supply an unapproved therapeutic good to a single patient
- The application must provide clinical justification for the use of the product
- This is the most commonly used pathway for accessing certain alternative treatments
SAS Category C
- Applies to specific therapeutic goods that the TGA has deemed appropriate for supply under this scheme
- Medical practitioners may supply these goods without individual approval, subject to certain conditions
It is important to note that SAS approval is not guaranteed. Each application is assessed on its merits, and the TGA may:
- Request additional information, or
- Decline applications that do not meet the required standards
Patients should understand that approval under the SAS does not constitute TGA endorsement of the therapeutic good or its efficacy. It simply provides a legal mechanism for access under medical supervision.
Authorised Prescriber Scheme
The Authorised Prescriber Scheme allows certain medical practitioners to prescribe specific unapproved therapeutic goods to a class of patients with a particular medical condition, without needing to seek approval for each individual patient.
This pathway is designed for situations where a medical practitioner has:
- Developed expertise in treating a specific condition with a particular therapeutic good, and
- Expects to treat multiple patients with similar needs
To become an Authorised Prescriber, a medical practitioner must:
- Apply to the TGA
- Demonstrate their qualifications and experience in treating the relevant condition
- Explain their rationale for using the specific therapeutic good
Authorised Prescribers are subject to:
- Ongoing reporting requirements
- Obligations to maintain appropriate records of their prescribing activities
The Role of Telehealth in Alternative Healthcare
Telehealth has emerged as a transformative force in Australian healthcare, particularly in the alternative healthcare sector. The ability to conduct medical consultations remotely has:
- Expanded access to specialised services for patients regardless of their geographic location
- Maintained the regulatory safeguards that protect patient safety
Evolution of Telehealth in Australia
Telehealth services in Australia have expanded dramatically, driven initially by necessity during the COVID-19 pandemic and subsequently by recognition of the benefits these services provide.
- Medicare rebates for telehealth services, originally introduced as temporary measures, have become an established part of the Australian healthcare system
- Patients can now access medical consultations from their homes
For alternative healthcare, telehealth offers particular advantages:
- Specialist practitioners with expertise in specific alternative treatments may be concentrated in major cities or specific regions
- Telehealth enables patients from anywhere in Australia to access these practitioners without the need for travel
- This reduces barriers to care and enables more patients to explore their healthcare options
What to Expect from a Telehealth Consultation
Understanding what happens during a telehealth consultation can help patients prepare effectively and engage meaningfully with their healthcare providers. While specific processes may vary between providers, most telehealth consultations follow a similar structure.
Before the consultation
Patients are usually asked to:
- Complete intake forms providing:
- Medical history
- Current medications
- Medical records
- test results
- medication lists
- reason for consult
This information enables the practitioner to prepare for the consultation and supports efficient use of appointment time.
During the consultation
The practitioner will typically:
- Discuss the patient’s health concerns
- Review medical history
- Conduct an assessment appropriate to the telehealth format, which may include:
- Discussing symptoms
- Reviewing previous treatments
- Exploring the patient’s goals for their healthcare
- Provide information about relevant options
- Discuss potential benefits and risks of different approaches
After the consultation
If treatment is recommended, the practitioner will explain next steps, which may include:
- Prescriptions
- Further testing
- Referrals to other healthcare providers
- Lifestyle modifications
Patients should receive clear information about:
- Follow-up arrangements
- How to contact the clinic with questions

Ahpra Guidelines for Telehealth
Ahpra has established clear guidelines for telehealth practice that apply to all registered health practitioners conducting remote consultations. These guidelines ensure that telehealth maintains the same standards of care as in-person consultations while acknowledging the unique characteristics of remote healthcare delivery.
Key principles of telehealth practice include:
- Clinical assessment standards
Practitioners must ensure they have sufficient information to make appropriate clinical decisions. If a telehealth consultation is insufficient for proper assessment, practitioners should arrange in-person review. - Informed consent
Patients must be informed about the nature of telehealth consultations, including any limitations compared to in-person care. - Continuity of care
Practitioners should ensure appropriate follow-up care and facilitate communication with the patient’s regular healthcare providers. - Documentation
Telehealth consultations must be documented with the same thoroughness as in-person consultations.
Making Informed Healthcare Decisions
Exploring alternative healthcare options requires careful consideration and engagement with qualified healthcare providers. Making informed decisions about healthcare involves:
- Understanding the evidence base for different treatments
- Considering personal circumstances and preferences
- Working collaboratively with healthcare providers to develop appropriate care plans
Questions to Ask Your Healthcare Provider
When discussing alternative healthcare options with a medical practitioner, patients may find it helpful to prepare questions in advance. Consider asking:
- What is the evidence base for this treatment option?
Understanding what research exists helps patients make informed decisions. - What are the potential benefits and risks?
Every healthcare intervention has both potential benefits and risks that should be understood. - Are there any interactions with my current medications or treatments?
This is particularly important for patients taking other medications. - What are the costs involved?
Understanding the financial implications of different treatment options helps patients plan appropriately. - What follow-up care is recommended?
Ongoing monitoring and support are important components of comprehensive healthcare. - What are the alternatives?
Understanding all available options enables patients to make truly informed choices.
Evaluating Health Information
Patients seeking information about alternative healthcare options encounter a wide range of sources, from peer-reviewed medical journals to social media posts. Developing skills to evaluate health information critically helps patients distinguish between reliable information and misinformation.
Consider the following when evaluating health information:
- Source credibility
Is the information from a reputable health organisation, peer-reviewed journal or qualified healthcare professional? - Evidence base
Does the information reference scientific research? Are claims supported by evidence rather than anecdotes? - Balance
Does the information acknowledge both benefits and risks? Claims that something has only benefits or no risks should be treated with caution. - Currency
Is the information current? Medical knowledge evolves, and older information may no longer reflect current understanding. - Conflict of interest
Is the source selling products or services? Commercial interests may influence how information is presented.
The Importance of Medical Supervision
Alternative healthcare options should always be explored under the guidance of qualified healthcare practitioners. Medical supervision ensures that:
- Treatments are appropriate for individual patients
- Potential interactions with other treatments are identified
- Patients have access to proper follow-up care
Self-treating with alternative therapies, particularly those involving therapeutic goods, can carry significant risks.
Healthcare practitioners bring expertise in:
- Assessing individual health circumstances
- Understanding the evidence base for different treatments
- Monitoring for adverse effects
They can also help patients:
- Navigate the regulatory pathways for accessing certain treatments
- Ensure that all care is provided within legal frameworks
Privacy and Patient Rights
Patients exploring alternative healthcare options in Australia are protected by robust privacy and patient rights frameworks. Understanding these rights helps patients engage confidently with healthcare providers and ensures their personal and medical information is handled appropriately.
Privacy Protection
Healthcare providers in Australia are bound by privacy laws that protect patients’ personal and health information. The Privacy Act 1988 and the Australian Privacy Principles establish requirements for how healthcare providers:
- Collect
- Use
- Store
- Disclose
patient information.
Patients have the right to:
- Access their own health records
- Request corrections if information is inaccurate
When engaging with telehealth services, patients should ensure they understand how their information will be handled. Legitimate healthcare providers will:
- Have clear privacy policies explaining data collection and storage practices
- Conduct telehealth consultations through secure, encrypted platforms that protect the confidentiality of patient information
Patient Rights
The Australian Charter of Healthcare Rights outlines the rights of patients in the Australian healthcare system. These rights apply equally to alternative healthcare services and include:
- Access – The right to healthcare services that address individual needs.
- Safety – The right to receive safe and high-quality care.
- Respect – The right to be treated with dignity and respect.
- Communication – The right to receive information in a way that is understood.
- Participation – The right to participate in decisions about healthcare.
- Privacy – The right to privacy and confidentiality of personal information.
- Comment – The right to provide feedback or make a complaint about healthcare services.
Costs and Practical Considerations
Understanding the financial aspects of alternative healthcare helps patients plan effectively and avoid unexpected costs. The cost structure for alternative healthcare services varies depending on:
- The type of service
- The provider
- Whether treatments are covered by Medicare or private health insurance
Consultation Costs
Medical consultations, including those for alternative healthcare, typically attract fees that may or may not be partially covered by Medicare.
- Telehealth consultations with medical practitioners may be eligible for Medicare rebates if they meet the requirements for Medicare-funded services.
- Patients should clarify fee structures when booking appointments, including whether any out-of-pocket costs apply.
Specialist alternative healthcare clinics may have different fee structures from general practice. Some clinics offer:
- Initial consultations that include comprehensive assessments
- Ongoing review appointments
Understanding the full cost structure, including any ongoing costs for follow-up care or monitoring, helps patients make informed decisions.
Treatment Costs
If treatment is recommended following a consultation, there may be costs associated with:
- Therapeutic goods
- Follow-up appointments
- Monitoring tests
Patients should discuss these potential costs with their healthcare provider before commencing treatment. Some treatments may require ongoing costs that should be factored into healthcare planning.
Private health insurance may provide coverage for some alternative healthcare services, depending on the specific policy and level of coverage. Patients should:
- Check with their health fund to understand what services are covered
- Review any applicable limits or waiting periods
Finding Reliable Healthcare Providers
Selecting appropriate healthcare providers is a crucial step in exploring alternative healthcare options. Patients should seek providers who are:
- Appropriately qualified
- Registered where required
- Transparent about their services and regulatory compliance
Verifying Practitioner Credentials
For practitioners in regulated health professions, patients can verify registration through the Ahpra public register. This register shows:
- The practitioner’s registration status
- Qualifications
- Any conditions or restrictions on their practice
Medical practitioners should be registered with the Medical Board of Australia.
For practitioners in professions that are not nationally regulated, patients should inquire about:
- Relevant qualifications
- Memberships in professional associations
- Any state-based registration requirements
Reputable practitioners will be transparent about their credentials and happy to discuss their qualifications with patients.
What to Look for in a Healthcare Provider
When evaluating healthcare providers offering alternative healthcare services, consider whether they demonstrate:
- Transparency
- Clear information about qualifications, services offered, fee structures and regulatory frameworks.
- Evidence-informed practice
- Recommendations based on available evidence.
- Willingness to discuss the evidence base for different treatment options.
- Patient-centred approach
.- Respect for patient preferences.
- Adequate information for informed consent.
- Involvement of patients in decision-making
- Appropriate referrals
- Willingness to refer patients to other healthcare professionals when appropriate.
- Regulatory compliance
- Demonstrated compliance with relevant regulatory requirements, including TGA regulations where applicable.
Conclusion: Navigating Your Healthcare Journey
Australia’s healthcare system offers patients access to a diverse range of therapeutic options, including alternative healthcare approaches that operate within robust regulatory frameworks designed to ensure patient safety. Understanding this landscape empowers patients to make informed decisions about their healthcare while engaging appropriately with qualified healthcare providers.
Key principles for navigating alternative healthcare options in Australia include:
- Understanding the regulatory frameworks that govern healthcare delivery
- Accessing treatments only through legal pathways and under medical supervision
- Engaging with appropriately qualified healthcare providers
- Making informed decisions based on reliable information and professional medical advice
Telehealth has expanded access to specialised healthcare services, including alternative healthcare, for patients across Australia. When conducted through appropriate platforms and by qualified practitioners, telehealth consultations provide a legitimate pathway for exploring healthcare options while maintaining the same standards of care as in-person consultations.
As you continue your healthcare journey, remember that:
- All healthcare decisions should be made in consultation with qualified healthcare practitioners
- Only a clinician who knows your medical history and current circumstances can provide individualised advice
The information in this guide provides a foundation for understanding the landscape of alternative healthcare in Australia, but it should not replace professional medical advice.
Learn More About Your Healthcare Options
To learn more about alternative healthcare pathways or to book a consultation with a qualified healthcare practitioner, contact our clinic.
Our team provides evidence-based information and guidance to help you make informed decisions about your healthcare.
- Book a consultation:
Learn More About Your Healthcare Options
Educational Disclaimer
This content is provided for educational purposes only and does not constitute medical advice, diagnosis or treatment recommendations. The information presented reflects current regulatory frameworks and general healthcare options available in Australia but may not capture the most recent regulatory changes.
Always consult with a qualified healthcare practitioner for advice regarding your individual health circumstances. Any treatment decisions should be made in consultation with appropriate medical professionals.
References and Further Reading
- Therapeutic Goods Administration (TGA) – www.tga.gov.au
- Australian Health Practitioner Regulation Agency (Ahpra) – www.ahpra.gov.au
- Australian Commission on Safety and Quality in Health Care – www.safetyandquality.gov.au
- Therapeutic Goods Act 1989 (Cth) – www.legislation.gov.au
- Australian Charter of Healthcare Rights – www.safetyandquality.gov.au/australian-charter-healthcare-rights
- World Health Organization – Traditional, Complementary and Integrative Medicine – www.who.int/health-topics/traditional-complementary-and-integrative-medicine
Last Updated: January 2026
Review Date: January 2027
